What The Health?! Woman fears excessive dancing caused her uterus to 'fall out'

Can leftover spaghetti really kill you? Can you actually cough up a blood clot in the shape of your lung? In Yahoo Lifestyle Canada‘s newest series, What The Health?!, we ask doctors to weigh in on odd health news stories and set the record straight. Be sure to check back every Friday for the latest.
A woman had to seek medical attention recently after her uterus reportedly slipped out of place and protruded out of her vagina while she was dancing.
The 60-year-old woman was shimmying during a dance workout in a public square in China when she felt as if something had “fallen out” of her body. According to Chinese video news site Pear, she immediately went to the Maternal and Child Health Centre in Xuzhou, Jiangsu Province in tears.
ALSO SEE: What The Health?! What you need to know about the deadly death cap mushroom
There, Dr. Song Hongjuan diagnosed the woman with uterine prolapse, a condition in which the uterus drops into the vaginal canal or even protrudes from it.
Although the woman feared she had caused the prolapse by “dancing too hard”, Dr. Song explained that in fact, it would have occurred because of the woman’s uterus being weakened from childbirth.
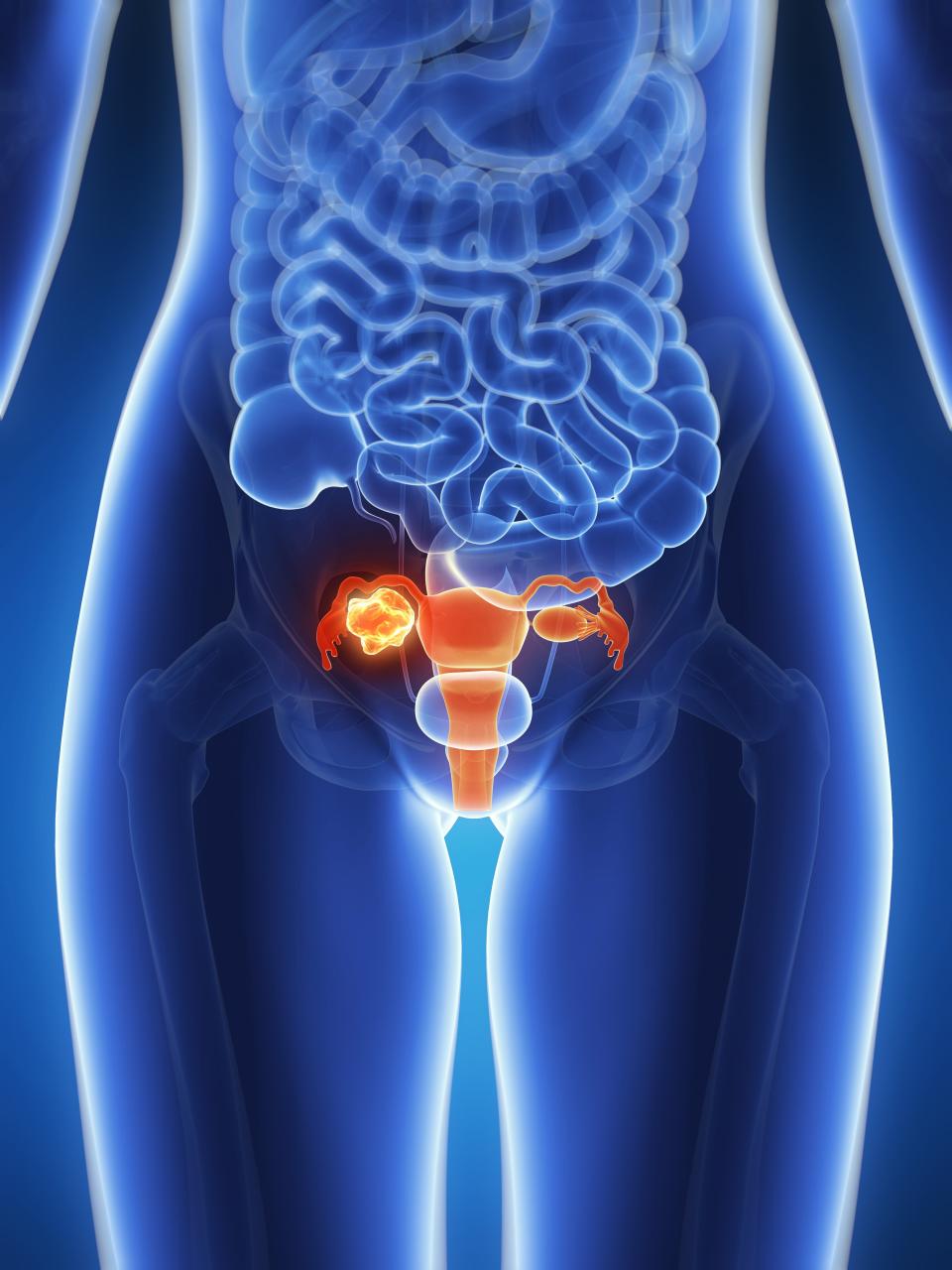
Besides the uterus, other organs in the pelvis can slip down from their normal position and bulge into the vagina. Called pelvic organ prolapse, it can be the bladder, bowel, or top of the vagina. When the entire uterus is outside the vagina, it’s called procidentia.
Pelvic-organ prolapse is more common than people may realize.
More than half of all women who have vaginal childbirth will develop some form of prolapse in their lifetime, explains Dr. Magnus Murphy, a urogynecologist founder of Calgary’s Pelvic Floor, a medical clinic that specializes in pelvic-floor disorders.
“It’s extremely common,” Murphy says. “Most women develop it in later life, after their 50s or even later, but it can happen in the 20s and 30s; it can happen very, very early.
ALSO SEE: Expert debunks mom medical myths with star of Netflix's 'Black Summer' Jaime King
“The overwhelming cause of prolapse is vaginal childbirth. The main reason is the injuries that are sustained during vaginal childbirth. These injuries aren’t readily apparent or noticed or diagnosed or known. The injuries could be to the muscles or to ligaments. Women start noticing something often decades later, although in more dramatic cases it can be pretty early.”
Childbirth isn’t the only association with the condition, Murphy emphasizes. Although rare, prolapse can also be linked with very hard physical labour or heavy lifting over a lifetime, connective-tissue disorders, or a hysterectomy without adequate suspension of the vagina post-surgery. It can also occur due to sarcopenia, the degeneration or weakening of muscle tissue, including that of the pelvic-floor muscles, as a natural part of the aging process.
Other risk factors include conditions that cause increased pressure in the abdomen or strain on the pelvic-floor muscles such as chronic cough (with bronchitis or asthma), repeated straining due to constipation, and being overweight or obese.
ALSO SEE: Hero nurses who helped care for AIDS patients in the 1980s featured in new documentary
It is not, Murphy says, caused by energetic dancing, as the woman in China feared.
“That’s just nonsense,” Murphy says. “Yes, a vigorous activity can precipitate a prolapse but it doesn’t cause the underlying deficiency that set you up for it. If you have strong pelvic-floor muscles, tough connective tissue, dancing is not going to cause a problem; it’s a lifetime of straining or micro trauma or it’s that acute, severe injury which heals with scar tissue, which gets weaker as you get older.”

Prolapse develops gradually, not instantaneously. Normally, the uterus is held in place just above the interior end of the vagina by a kind of hammock made up of muscles and ligaments. Wear and pressure on these supportive pelvic structures can allow the bottom of the uterus (or the floor of the bladder or both) to sag through them.
Mild cases of uterine prolapse often don't cause any symptoms. A sign of more advanced prolapse is discomfort in the vagina, pelvis, lower abdomen, groin or lower back, often described as an aching or pulling sensation, which can be worse during sex or menstruation.
ALSO SEE: It seems like Alzheimer's but peek into brain shows a mimic
Heaviness or pressure in the vaginal area can also be a sign. Some women feel like something is about to fall out of the vagina, while others describe it as the feeling of sitting on a small ball.
Another symptom is a bulge of moist, pink tissue from the vagina. This exposed tissue may be irritated and cause itching or small sores that can bleed.
Other signs include leakage of urine, which can be exacerbated by heavy lifting, coughing, laughing, sneezing, or sex; pain during sexual intercourse; difficulty having bowel movements; discomfort while walking; and discharge that soils your undergarments.

There are various forms of treatment for prolapse, with surgery only being suggested for extreme cases, Murphy says.
“Surgery is not all it’s cracked up to be,” he reveals. “The failure rates are extremely high. The end result is not a perfect vagina. That doesn’t mean surgery doesn’t work, but you have to have realistic expectations. If you have a mild or minimal prolapse, you might be disappointed.
“If your prolapse is outside your vagina—the worst type of prolapse could be 10 centimetres down from the opening of the vagina; it can be completely out, completely inverted, so your entire uterus and bladder, everything, is outside your body—then I can say the chances you’ll be better after surgery is 100 percent, unless you get some bad complications. If you have a prolapse that’s still inside vagina, then your likelihood to have better off after surgery is significantly reduced.”
ALSO SEE: 'Ketosis is a state of medical emergency': Jillian Michaels slams keto diet — yet again
Other approaches include treating muscle atrophy with estrogen or laser, or the use of pessaries. Made of medical-grade rubber in various shapes and sizes, they’re placed inside the vagina like a tampon to occupy the space and prevent anything from falling out. They can stay in for three months then need to be cleaned. There are also cloth versions, which must be replaced every eight hours.
The downside of these devices is that they interfere with spontaneous sexual activity, mask urinary incontinence, and can cause discharge or erosion, the latter which Murphy describes as a kind of pressure sore.

Sometimes, elderly women who are done with sex can have a minimally invasive surgery to close the vagina.
Murphy encourages women to stop smoking and lose weight or maintain a healthy weight to reduce the risk of prolapse. It can also be prevented by exercising the muscles of the pelvic floor.
ALSO SEE: Mum urges parents to vaccinate their children, shares photos of her newborn with measles
“Pelvic-floor physiotherapists are your best friend, even more important than your doctor,” Murphy says. “You don’t see the effect of pelvic-muscle action; this is why they’re neglected muscles. But they’re huge muscles and they’re hugely important, because they have a function with everything that goes on down there: sexual function, evacuation of bladder and bowels, and continence of bladder and bowels. Women need to be aware of the importance of them.”
For women who are noticing prolapse and freaking out, Murphy has some reassuring words.
“It’s common, but don’t panic,” he says. “You’re not the only one. Don’t be embarrassed about it, and don’t be ashamed of it. Your life’s not over. We can treat it. Physiotherapy is a good place to start.”
Let us know what you think by commenting below and tweeting @YahooStyleCA!Follow us on Twitter and Instagram.
Check out Yahoo Canada’s podcast, Make It Reign — our hot takes on all things royals in a non-stuffy way — on Apple Podcasts and Google Podcasts.



